Last updated on September 14th, 2023
Insulin doses are put on a chart named sliding scale. The physician generates this insulin chart with the help of the patient. A chart is prepared on how the individual’s body reacts to insulin, their everyday routine, and carbs consumption that they would consent to. Insulin doses differ based on two factors:
- Pre-meal levels of blood sugar: This generally arises on the left side of the Novolog sliding scale chart, from low to high, with higher insulin dosages toward the bottom of the scale. The higher the blood glucose an individual has, the greater the amount of insulin people would require to cope with it.
- Mealtime insulin dosing: This generally arises along the scale’s top row. This top row indicates breakfast, lunch, and then dinner.
The dose of insulin changes all through the day; this is due to insulin sensitivity. Insulin sensitivity is how the body reacts to insulin, which may alter throughout the day. The meal composition also modifies during the day, and the physician may keep it in mind.
Also Read: Fasting Blood Sugar Levels Chart

Ways to Determine Dosage of Insulin

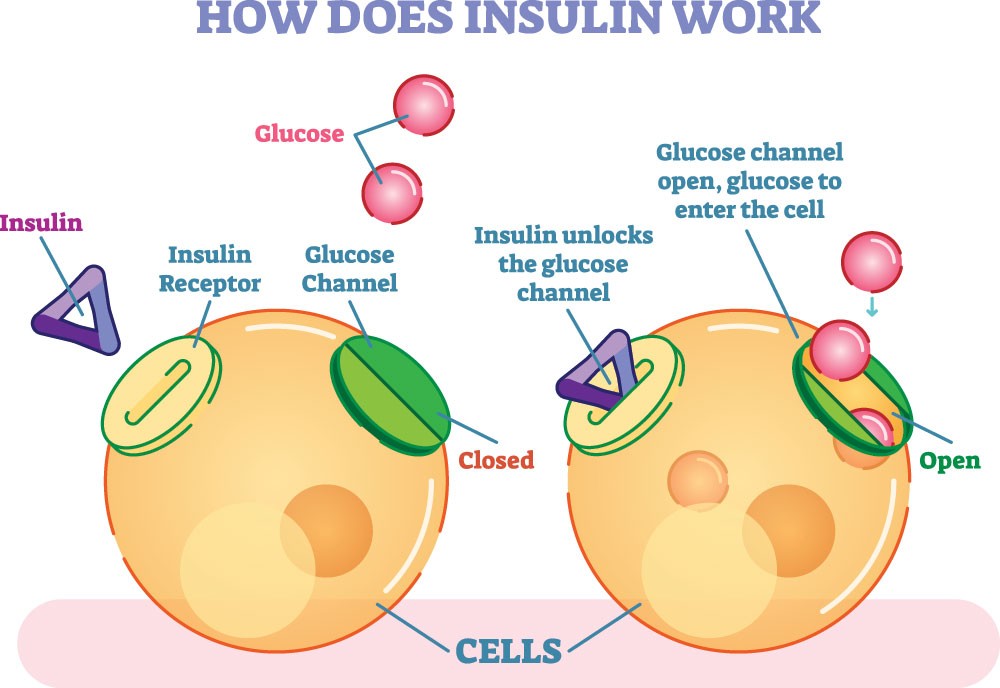
Insulin is the groundwork of treatment for a majority of people with diabetes. If a person has diabetes, their body either fails to produce sufficient insulin or effectively makes use of insulin. Individuals with type 1 diabetes and a few individuals with type 2 diabetes ought to take numerous injections of insulin each day. Insulin normalises blood glucose and avoids spikes in glucose levels. This also assists in preventing complications. The insulin amount a person can take can be determined in different ways:
- Fixed-dose insulin: According to diabetes.co.uk, a definite set amount of insulin units are taken in this method at each meal. For instance, the person can take six units at breakfast and eight at dinner. The numbers don’t modify depending on the person’s blood glucose readings or the food quantity consumed. Whereas this might be simpler for individuals just beginning insulin, it doesn’t answer for levels of pre-meal blood glucose. In addition, it doesn’t factor in the varying quantities of carbs in a particular meal.
- Carb-to-insulin ratio: In this sliding scale approach, a person takes a particular quantity of insulin for a specific amount of carbs. For instance, if a person’s breakfast carb-to-insulin ratio is 10:1 and they consume 30 grams of carbs, they can take three units before breakfast to cover the meal. According to the NLM, here is a detailed explanation of the carb-to-insulin ratio for type 1 diabetes patients who use insulin pumps.
- Sliding-scale insulin therapy (SSI): As per the National Institute of Health, in this approach, the dose depends upon a person’s blood glucose level just before having food. The higher the blood glucose levels, the more insulin they can use. The therapy can be primarily used in hospitals and other healthcare facilities as it’s often simple and handy for the medical staff to manage.
Also Read: Energy Drinks For Diabetics

What’s a Sliding Scale Therapy and How does it Work?
In most sliding-scale insulin therapy regimens, the patient’s glucose levels in the blood are taken with the help of a glucometer. This can be performed around 4 times per day (every five to six hours, before meals and at bedtime). The quantity of insulin a person can receive at mealtime depends upon their glucose values. In many cases, fast-acting insulin can be used.
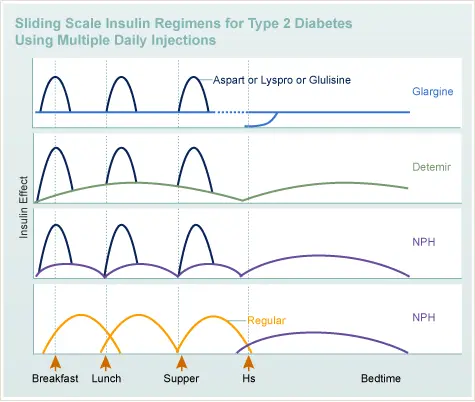
Sliding Scale Insulin Regiments For Type 2 Diabetes Using Multiple Daily Injection
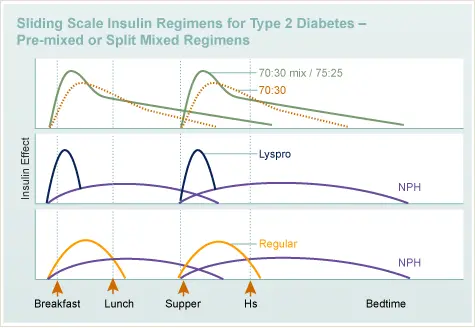
Sliding Scale Insulin Regiments For Type 2 Diabetes – Pre-mixed or Split Mixed Regiments
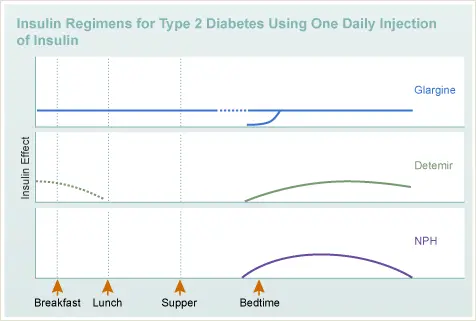
Insulin Regimens for Type 2 Diabetes Using One Daily Injection of Insulin
Reading the Sliding Scale Insulin Chart
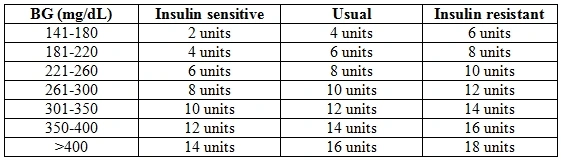
How to calculate insulin dose based on blood sugar? To work out the appropriate dose of insulin with a sliding scale, some steps should be followed:
- Blood sugar levels should be tested.
- A matching blood sugar value should be matched along the type 2 diabetes insulin dosage chart’s left column.
- Slide horizontally along that value’s row until the current meal is reached.
- A dose that corresponds to the number where the two values meet should then be taken.
The individual must test their blood glucose levels before mealtime based on the type of insulin they utilise. Various insulin types work more than varied time durations. According to the NHS, if an individual utilises rapid-acting insulin, they can take their insulin 10-15 minutes before having food. In addition to these mealtime rapid-acting doses, individuals repeatedly take a long-acting insulin dosage one time or two times each day.
Also Read: Lowering Blood Sugar Level Naturally
Also Read: HbA1c Normal Range Chart
Pros and Cons of Sliding Scale Insulin

The sliding scale means a small number of daily calculations. People with diabetes might feel more relaxed following a pre-determined plan. On the other hand, these factors also make this type of treatment rigid.
- Timing of the meal: An individual is required to consume their meals around the same time daily. If they are not following this, their insulin sensitivity might not go with the ones the chart utilises to work out the dose for a particular meal.
- Nonflexible routine: The method demands a specific diet regimen and exercise plan to succeed.
- Carbs: An individual should take a similar number of carbohydrates with each meal, as the chart’s calculations are based upon a single carbohydrate value. This number must not alter each day.
- Exercise: People must not change the intensity of their exercises daily. Modifications in stress and physical activity also have an effect on blood sugar levels in a way that the sliding scale is unable to answer for.
On the other hand, it is hard for many individuals to follow these meals as well as activity restrictions wholly as the sliding scale does not permit modifications in carb consumption, meal timings, and exercise. Consequently, considerable alterations in blood sugar levels may take place all over the day. Medical experts are also anxious that the sliding scale has some risks of constant high sugar levels.
High blood glucose: According to studies published in the American Diabetes Association, using a sliding scale failed to improve sugar control, but it caused more recurrent high blood glucose or hyperglycemia signs.
Low blood sugar: The doses that appear on a chart may also be too many if an individual misses out on meals or is more susceptible to insulin on a certain day. As these dosages accumulate during the day, they might bring about a hazardous fall in blood sugar levels. This may hastily turn out as a serious emergency, leading to coma and perhaps death.
Also Read: Benefits of Sabja Seeds
Alternatives of Sliding Scale Insulin
Instead of the sliding scale model, the ADA suggests other methods of using insulin.
Conventional Insulin Therapy
This treatment includes injections of the following:
- Long-acting insulin: One dose per day. To make this method effective, the individual should consume their meals at the same time on a daily basis, or unnecessary variations in blood sugar may be the result. Here is detailed information on how to use long-acting insulin according to the diabetes.co.uk.
- Short-term insulin: An individual takes two to three doses daily and should systematise their meals with the peak activity times of the injections. The daily doses are similar and fail to count on pre-meal blood sugar levels.
Insulin Pens
An individual can utilize an insulin pen to inject insulin. These pens are modifiable so that different doses can be injected at the same time. This pen is quite simple for use as compared to a syringe. It is available in the form of a prefilled or refillable device.
Intensive Insulin Therapy
This therapy includes 3 types of insulin doses. This means is also called basal-bolus therapy or tight control. An individual must make daily calculations to keep their sugar levels as close to their intended level as they can. The therapy balances in real-time for factors that have an effect on blood sugar levels and insulin sensitivity. To compute this dose, an individual works on the variation between their target glucose level as well as their current level, however, the amount of additional glucose is currently present. After that, they will take a sufficient amount of insulin to process the added glucose. The therapy is found to be effective if an individual follows it appropriately, but can be difficult to use.
Also Read: Diabetic Gastroparesis Symptoms
Pros and Cons of Insulin Pump Therapy
A lot of individuals who require insulin make use of an insulin pump. It has the same mechanism of action as basal-bolus insulin, but it eliminates the necessity for regular injections. An insulin pump is a small, digital device offering a steady supply of insulin all over the day (basal), with an added dose around meal times (bolus). The individual requires wearing the pump on their body. The pump makes sure that insulin travels through it, via a small tube as well as a needle, into the body. A person will be required to work with their physician to program the pump as well as to work out which doses they require. They might still require injecting insulin at mealtimes or after doing physical activity. They will also require checking their sugar levels on a regular basis, just like other means of insulin therapy.
Also Read: How to Test Diabetes at Home?
Problems with Sliding-Scale Insulin Therapy
There are some concerns about using sliding-scale insulin therapy. These may be:
- Diet: What a person consumes greatly affects the requirement for insulin. For instance, if a person consumes a diet rich in carbs, then a higher dose of insulin is needed than if a person eats a low-carb diet.
- Weight factoring: How to calculate insulin dose based on weight? An individual with more weight might require more insulin. Whether the person’s weight is 120 pounds or 180 pounds, every person can get the same dose. Individuals weighing 180 pounds cannot get adequate insulin to lower their blood glucose levels.
- Insulin history: The dose doesn’t explain the amount of insulin a person might need in the past. Also, it fails to consider how sensitive the person’s body is to insulin’s effects.
Summary
Effective blood sugar management is a great way to prevent complications from developing. It also assists individuals to live a longer as well as a healthier life. For an effectual low-dose regular insulin sliding scale therapy, the person requires a predictable and consistent lifestyle.
FAQs (Frequently Asked Questions)
Diabetic coma may occur when your blood glucose gets too high, 600 mg/dL or more, making you more dehydrated. It frequently affects individuals with type 2 diabetes that isn’t well-controlled.
To make better your glycemic control in diabetics; 500 units of insulin is for use in patients demanding above 200 units of insulin each day.
1 unit of insulin must reduce your blood glucose level 30-50 mg per dL, but you might require more insulin to attain a similar effect.
Diabetics who are hyperglycemic or with hospital-associated hyperglycemia are incapable of consuming oral fluid or foods, who are extremely in poor health, and/or for whom modification of their insulin regimen is not achievable.
Disclaimer
This site provides educational content; however, it is not a substitute for professional medical guidance. Readers should consult their healthcare professional for personalised guidance. We work hard to provide accurate and helpful information. Your well-being is important to us, and we value your feedback. To learn more, visit our editorial policy page for details on our content guidelines and the content creation process.

 English
English