Last updated on August 30th, 2022
Diabetic maculopathy is a medical problem that may occur due to retinopathy. Maculopathy is another term for macula damage. The macula is the part of the eye which offers a central vision. It plays a key role in fine vision (reading, writing, watching TV, comprehensive work, and identifying faces). A common form of damage happens because of diabetic macular oedema (DMO). In this condition, fluid accumulates on the macula. Often, treatment of this condition is by laser surgery.

What is the Retina?
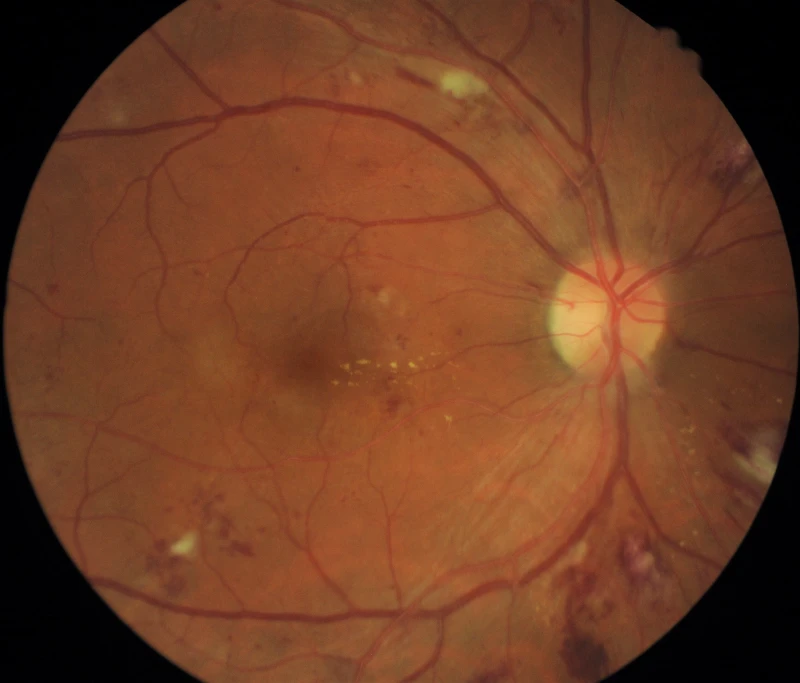
The retina is the layer of the eye that lines the backside of the eyes. Light goes in the eye and travels via the eye lens. The lens concentrates the light over the retina. Then, the messages regarding vision pass through the retina to the optic nerve and then towards the brain. There are several small blood vessels present adjacent to the retina that carries oxygen and nutrients to the retina cells.
Also Read: Can Diabetics Eat Fish?

What is Diabetic Maculopathy?
A diabetic maculopathy is a form of diabetic eye ailment that affects the macula. In this, the blood vessels that expand to make up for clogged blood vessels start leaking. Maculopathy happens when the leaked liquid accumulates on the macula and leaks into the retina resulting in inflammation. It results in the narrowing of the blood vessels present in the macula. Hence, the macula becomes short of oxygen and nutrition resulting in a worsened vision. The condition is termed ischaemic maculopathy.
Also Read: Best Home Remedies to Cure Diabetes
Diabetic Maculopathy Symptoms
The signs of diabetic maculopathy may include blurry central vision. This might be observed by:
- Identifying faces in the centre of vision
- Difficulty while reading
Diabetic Maculopathy Diagnosis
Diagnosis of macular oedema occurs by clinical assessment by an expert ophthalmologist (eye specialist). At times, there is a need for extra information for evaluating the most appropriate treatment choices. Also, there might be a need for a fluorescein angiogram test.
Also Read: Best Yoga To Control Your Diabetes
Treatment of Diabetic Maculopathy
The goal of treatment is to stop the leakage of the blood vessels. Laser treatment and injectable medications like anti-vascular endothelial growth factor (Anti-VEGF) are most appropriate. These injectables are given in the eye and nowadays these are the standard treatment for diabetic maculopathy. Other intervention options may involve steroid injections of Ozurdex or Iluvien.
Also Read: Symptoms of Diabetes
Diabetic Maculopathy and Laser Treatment
The major objective of this treatment is to stabilise the changes within the eye that result due to diabetes. The treatment does not result in a visual improvement, though in a few cases it may improve too. Yet, it is possible that in the absence of this treatment, a person would lose all or some of the vision.
How the Treatment is Done?
The laser treatment is done by an intense light beam on the retina in small spots. The application of mild laser burns is done on the central part of the retina. A person may require much less laser treatment in comparison to other diabetic retinopathy.
What are the Risks Involved in the Treatment?
Maculopathy treatment involves very rare complications. These are:
- Around 1 in 10 individuals report a little, however a permanent blind spot adjacent to the centre of their sight.
- Few individuals may notice the laser pattern post-treatment. This generally carries on for up to 2 months and rarely for up to 6 months post-treatment.
- The probability of a person losing most of his or her central vision months or years post-laser treatment is below 1 in 300 (0.3%).
- Also, the treatment involves a slight risk of unintentional laser burns to the centre of the vision. This may occur if a person faces difficulty in staying still or unintentionally looking directly at the laser as it fires.
- Rarely, months or years post-treatment, a laser burn on the retina might give rise to the production of new blood vessels under the macula. These may bleed and scar up bringing about a lasting loss of the central vision.
Also Read: Indian Diet Plan For Diabetes Type 2
What are the Benefits of Receiving the Treatment?
The goal of maculopathy treatment is to prevent an additional loss of sight. Even if a few people have restored their vision, medicines might not bring back vision that has already been lost. Also, it might not eventually stop further loss of vision resulting because of an ailment.
Unfortunately, liquid in the macula region returns and requires re-treatment so as to not lose control over the ailment. The treatment is expected to begin with five injections at 4 weekly intervals. After that, a person would be evaluated for the treatment response. If a person responds well to the treatment, then he or she can extend the intervals to 2 monthly or 6 weeks based upon the medication or the response.
Summary
At times, the leak requires more than one laser treatment. These leaks are known as ‘macular oedema’. These are the regions of the thick spongy retinas. Many people having macular oedema require a laser.
Also Read: Top Homeopathic Medicines For Diabetes
Take Care of the Levels to Control Diabetic Maculopathy
By maintaining the levels as much as possible (or lower), a person does his or her best to stop the deterioration of the eyes. By adhering to the below-stated targets, retinopathy has been found to improve, even without laser.
Lifestyle
- Moderate alcohol intake. Limit the alcohol to one drink or unit a day, 6 days a week. Alcohol in excess may lead to brain damage.
- Half an hour to two hours of exercise in a day.
- Avoid obesity if required.
- A healthy diet involving nine portions of veggies or a few diabetic fruits a day (9 for males, 7 for females).
- Also, the diet must contain a negligible amount of animal or ‘hard’ veggie fats, and low salt as well.
- People can take oily fish like sardine, salmon, tuna, and trout, at least two times a week.
- A diabetic diet must include lots of fibre and healthy fats. They help in slowing down retinopathy. Avoid saturate and trans-fat.
- No refined or processed foods. They lead to weight gain and may cause inflammation all over the body.
Also Read: Madhunashini Vati For Diabetes
Blood pressure
- Standard blood pressure is 130/80 or rather less BMJ 16. Even less can work like 120/75.
- BP 125/75 or less if the protein is present in the urine present.
- Heart medications such as ACE inhibitors or ARBs are poorly tolerated in pregnant or very low blood pressure females.
- Depression and anxiety are responsible for increased blood pressure.
Sugar Levels
-
- 5.0 to 7.2 mmol/l prior to meals
- Less than 10.0 mmol/l after meals
- For people who test their sugar levels and adjust insulin doses, a recent glucose sensor is highly advisable. They are advantageous for type 1 diabetic patients.
Also Read: CRP Normal level Chart For Adults
HbA1c
- HbA1C value in the range of 6.5% to 7.5% or below with some or rather no hypos. These (or somewhat lower) levels are most suitable to avoid complications.
- HbA1C of 7.5% for insulin users; less than 6.5%, if people do not use insulin and have good health. The target must be adjusted as per a person’s age and health. If a person is a type 1 diabetic and does not reach good control, he or she needs checks for other health problems like celiac disease, thyroid disease, and Addison’s.
- If hypos occur, look out for expert advice from a diabetes specialist.
An Instant Reduction in HbA1c levels
- An unexpected improvement in the blood glucose regulation (HbA1c fall of 3%) would cause a brief rise in the development of retinopathy. Hence, a laser might be essential.
- Good blood sugar management is essential in the long run. That is post 2 years. When individuals who regulate their high blood sugars regulate their condition well would be better off after this time.
- A brief increase in retinopathy occurs most commonly while commencing insulin for the initial time, chiefly if the diabetes is poorly regulated while beginning insulin.
Statins and Cholesterol
- Less than 4.0mmol/l, and statins are advisable for many adults having diabetes regardless of their cholesterol levels.
- Statins are essential regardless of cholesterol levels if well-tolerated age more than 40 years. Statins lower the stage of retinopathy.
- A fibrate including fenofibrate might help in the case of any exudates.
- Avoid the medication if pregnant, with a GFR of less than 15, or with pancreatitis.
- If GFR is low but still is more than 15, a person might require a lower dose.
Insulin
- Type 1 diabetics and type 2 patients making use of insulin with considerable glucose variations, glucose sensors are good. These include Freestyle or Dexcom.
- Insulin pumps usually give an improved control and still are difficult to use.
Smoking
- Smoking increases the risk of retinopathy three or four times.
- Passive smoking might double the risk of retinopathy.
- Electronic cigarettes are much safer and perhaps carry an insignificant effect on the retinopathy.
- Just a cigarette each day increases the risk of heart problems, hence it is best to stop it totally.
Sleep apnoea
- This adds to macular oedema and loss of vision and many other serious issues.
- It is most common in people with diabetes, especially if they are obese or overweight. When it occurs in diabetics, it is diabetic macular oedema.
Glitazones
People can’t use Rosiglitazone and Pioglitazone if there is considerable retinopathy. Also, the medications are not safe in case of macular oedema as they augment fluid retention.
Early Maculopathy and Laser
The laser was formerly the major treatment, however, now it is being replaced with anti-VEGF injections. Areas of leakage may occur in the retina, and the retina may turn wet similar to a sponge. Leakage may develop resulting in more and more damage. In case of small regions of leakage, the laser may seal or decrease the leakage and prevent it from resulting in more damage.
An ophthalmologist may detect the leakage by assessing the eye on a ‘slit lamp’ in the health centre or utilizing an OCT. A laser is a very bright light and a very focused one. Hence, it produces tiny burns on the retina. The burns are so small that they result in a little damage while curing this form of maculopathy.
Also Read: Can Diabetics Eat Jaggery?
Summary
Mild oedema might calm down without a laser. Instead, an OCT photograph might be useful for measuring an increase in oedema and sight might worsen. The leakage is expected to lower if other things like sugar levels, blood pressure, smoking, and cholesterol levels get regulated.
So, is it possible to stop diabetic retinopathy from developing? Anybody can lower his or her risk of progressing diabetic retinopathy by keeping their glucose levels, blood pressure and cholesterol levels controlled. And, for this Breathe Well-Being is a great platform. Breathe Well-being Diabetes Reversal Plan can help and guide you through the entire thing. Type 2 Diabetes is no longer a lasting health condition. Diabetes reversal may cause improvement in the lifestyle of an individual. Also, it may aid in decreasing medical costs. The research-based reversal platform at Breathe Well-being helps a person lose weight to reverse the condition. It meaningfully improves a person’s standard of living and reduces their medical expenses as well!
FAQs:
References
- https://www.uhcw.nhs.uk/download/clientfiles/files/Diabetic%20Maculopathy%20and%20Treatment%20Options%20for%20Patients%20(1048)%20.pdf
- http://www.diabeticretinopathy.org.uk/diabetic_maculopathy.html
- https://www.diabetes.co.uk/diabetes-complications/diabetic-maculopathy.html
Last Updated on by Dr. Damanjit Duggal
Disclaimer
This site provides educational content; however, it is not a substitute for professional medical guidance. Readers should consult their healthcare professional for personalised guidance. We work hard to provide accurate and helpful information. Your well-being is important to us, and we value your feedback. To learn more, visit our editorial policy page for details on our content guidelines and the content creation process.

 English
English