Last updated on September 30th, 2022
When a person is diabetic, skin problems can be the initial symptom indicating the same. Diabetes has an impact on almost every body part, including the skin. Many diabetics experience a skin problem caused or tormented by diabetes at some time. Most common examples of these conditions may involve itching, fungal or bacterial infections. On the other hand, diabetics are more prone to complications such as diabetic dermopathy, eruptive xanthomatosis, necrobiosis lipoidica diabeticorum, and many others. Read further to know more about diabetes and skin problems associated with it and does diabetes causes skin infections.

Diabetes and Skin Problems
Diabetes can have an effect on any body part, including the skin. When skin gets affected by the ailment, it often indicates that there is a raised level of sugar in the blood. Diabetes causes itchy skin. This can signify either the person has undiagnosed diabetes, or pre-diabetes, or his or her diabetes treatment needs a modification.

Causes of Diabetic Skin Conditions
- Chronic diabetes type 2 with hyperglycemia (high blood sugar) is expected to be linked to poor blood circulation. This decreases the blood flow to the skin. In addition, it can result in damaged nerves and blood vessels. Also, when there are raised sugar levels, it leads to a reduction in the ability of the WBCs to resist infections.
- When blood circulation reduces, alterations in the skin’s collagen can be seen. This alters the texture, exterior, and healing power of the skin.
- When skin cells get damaged, it can even retard the sweating ability. Also, it can lead to an increased sensitivity to pressure and temperature.
- A reduction in sensation can be seen when a patient suffers from diabetic neuropathy. This can make the skin more susceptible to wounds that may not be visible and later on can be felt.
Also Read: How to Lower Your Blood Sugar Level?
Type of Diabetic Skin Conditions
Bacterial infections
Diabetics most commonly suffer from bacterial infections including:
- Boils
- Infections around the nails
- Styes (infections of the eyelid glands)
- Carbuncles (deep skin infections and infections of the underlying tissues)
- Folliculitis (infections of the hair follicles)
Inflamed tissues are generally red, hot, bloated, and aching. Numerous bacteria can cause such infections, the most common being Staphylococcus. Most bacterial infections need antibiotic treatment in the form of pills and/or creams.
Diabetics are more prone to bacterial infections than other people according to research. People with diabetes can lower down their probability of skin infections if they take care of their skin and follow a good skincare routine. It is a must to visit a doctor if any diabetic person notices such infections.
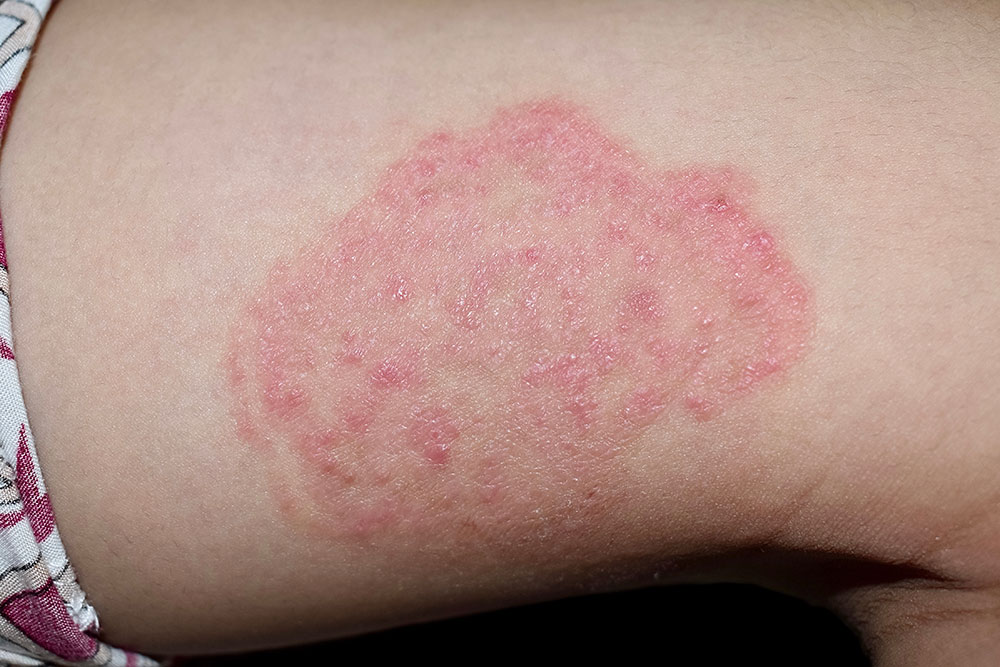
Fungal infections
Candida albicans is the culprit of fungal infections in type 2 diabetics. It is a yeast-like fungus and can form prickly rashes, tiny blisters, or scales. This fungal infection most commonly happens in moist, warm folds of the skin; regions beings, breasts, between fingers and toes, armpits and groin areas, around the nails, mouth corners, and under the foreskin.
Some of the common infections due to fungus may include ringworm, jock itch, vaginal infection, and athlete’s foot and these are responsible for itching. If any diabetic person believes he or she has yeast or fungal infection, it’s always a good idea to discuss it with the concerned doctor.
Also Read: Blood glucose converter
Itching
Diabetes often results in localized itching. The itching skin is also known as pruritus. The reasons can be poor blood circulation, yeast infection, or dry skin. When itching is because of poor circulation, then the most irritable regions can be the lower parts of the legs. It can be easily treated by practicing good hygiene, limiting the frequency of bathing in low humid conditions, or avoid hot showers. Also, it’s good using mild soap with moisturizer (keeps the skin moist and soft) and applying a skin cream after taking bath. Lotions or creams are effective in treating irritated skin.
Vitiligo
Vitiligo has an effect on the coloration of the skin. In this condition, the cells that make pigments get destroyed. This results in the formation of diabetic dry skin patches and discolored patches. The skin condition most commonly affects the hands, elbows, and knees; however, it can occur on the face (around the mouth, eyes, or nostrils). Vitiligo occurs in individuals with type 1 diabetes. Usage of a proper sunscreen (SPF of 30 or higher) must be done to prevent sunburns on the discolored skin.
Hypersensitive reactions
Various allergies to foods, medications, or bug bites can result in developing bumps, rashes, or depressions on the skin. Serious hypersensitive reactions may also need emergency treatment. Diabetics need to check for rashes or bumps in the regions where insulin is injected by them.
Also Read: Metsmall 500 tablet uses
Other Medical Conditions
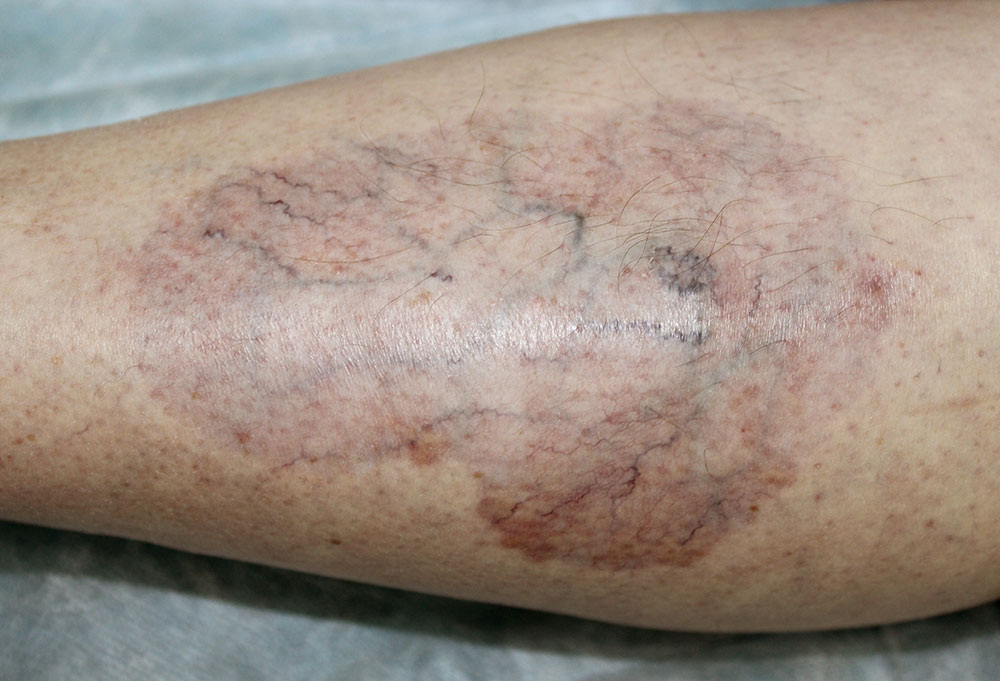
Necrobiosis Lipoidica: Yellow, Red, or Brown Patches on the Skin
Initially, small raised solid bumps appear on the skin just like pimples. These can also be called diabetes bumps. With progression, these bumps become patches of rough and inflamed skin. The appearance of such rough, reddish, and inflamed patches on legs is a condition called necrobiosis lipoidica.
Also, the person can notice:
- Blood vessels
- A shiny porcelain-like appearance on the surrounding skin
- Skin turning painful and itchy
Prevention:
- Get the sugar levels tested if any person has not been diagnosed.
- Discuss with the doctor about the way to better control the ailment.
- Check with a dermatologist about the skin. Necrobiosis lipodica is risk-free, but it might cause complications.
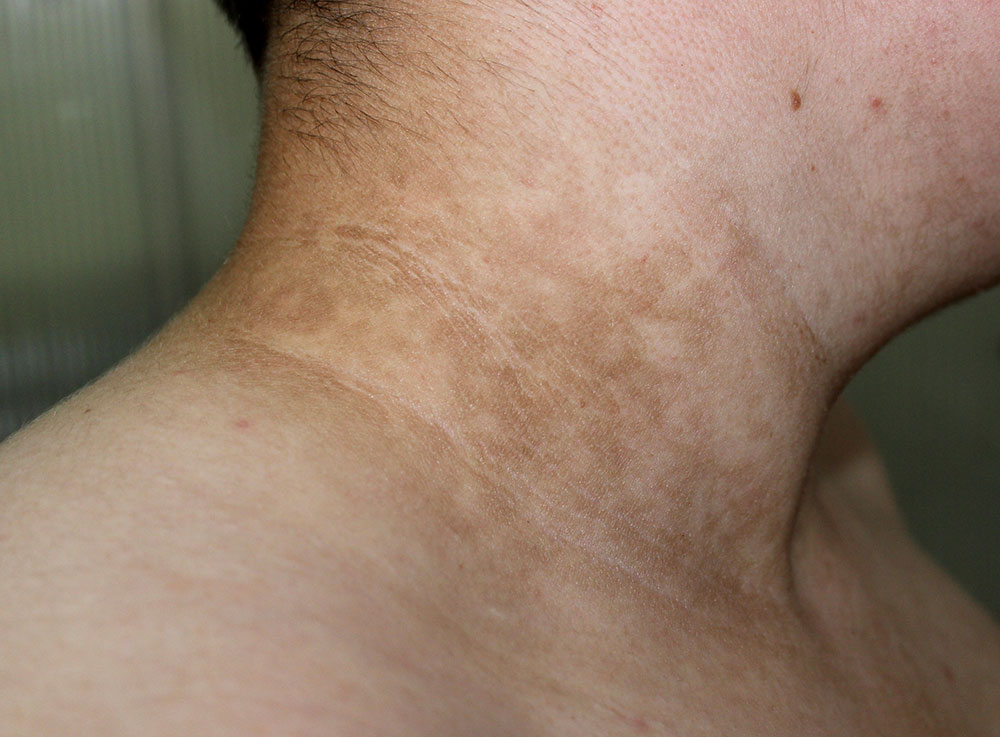
Acanthosis Nigricans: skin darker areas feeling like a velvet
In this condition, a dark patch of velvety skin appears on the areas like the armpit, back of the neck, or groin. This indicates that the person has an excess of insulin in his or her blood (dark patches on the skin due to diabetes). Frequently, this is a sign of prediabetes.
Prevention
Get tested for diabetes.
Digital Sclerosis
Digital sclerosis means Hardening and thickening of the skin
This skin condition develops on the fingers, toes, or both.
Also, the person may notice firm, waxy skin on the back of the hands. It can turn the fingers to become inflexible and their movement becomes difficult.
It is also seen that this tough, thick, and inflamed skin can spread to the upper arms and forearms. Also, the disease can develop on the neck, upper back, as well as shoulders; and at times the thickening skin can spread to the chest, face, or shoulders. This skin problem generally occurs in people with diabetic complications that are hard to treat.
Prevention:
- It’s always a good idea to discuss with the concerned doctor the thickening of the skin.
- Keeping diabetes under control also brings considerable relief.
- Also, the person can need physical therapy. When the skin of the finger, toe, or other joint areas gets thickened, physical therapy can only assist the person in bending and straightening the joint.
Also Read: Is watermelon good for diabetics?
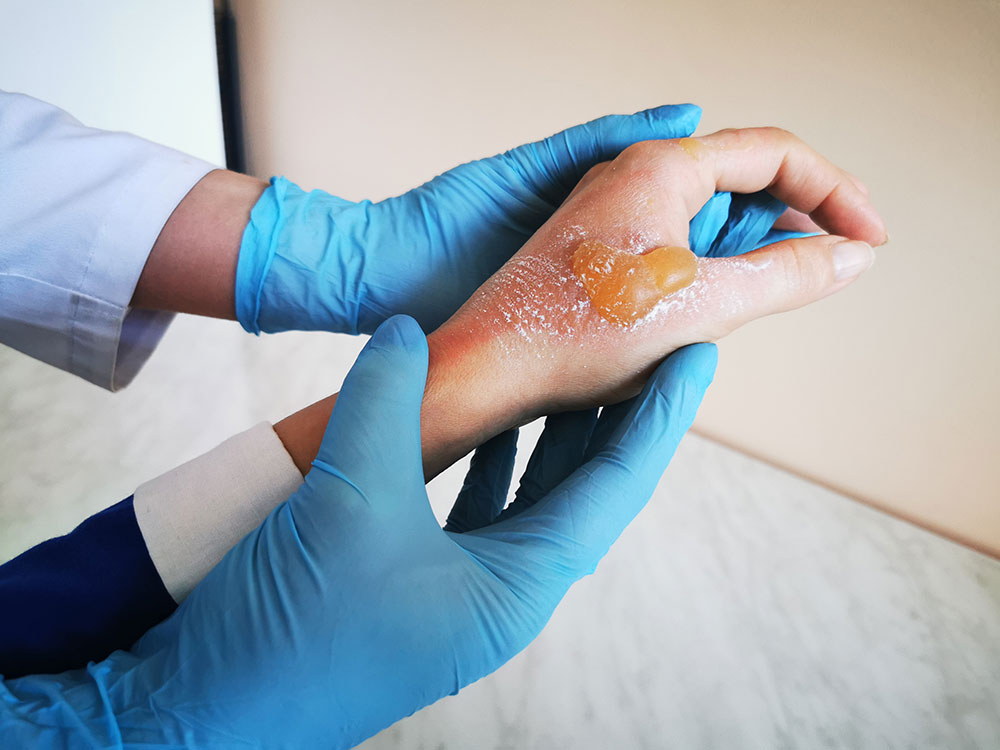
Bullosis Diabetricorum: Large Blisters
It is a rare skin condition but diabetics can see blisters unexpectedly emerging on their skin. A large blister can be observed, or a group of blisters can appear. These can appear on feet, hands, forearms, or legs. These blisters are somewhat the same in appearance as the blisters that emerge after a severe burn. But these blisters are not painful. Large blisters like these may appear on the diabetic’s skin. These are often called diabetes spots on the feet.
Prevention:
- Inform the healthcare provider about the blisters. It’s important to take the necessary steps to avoid an infection.
- Discuss with the doctor how to better control the blood sugar levels.
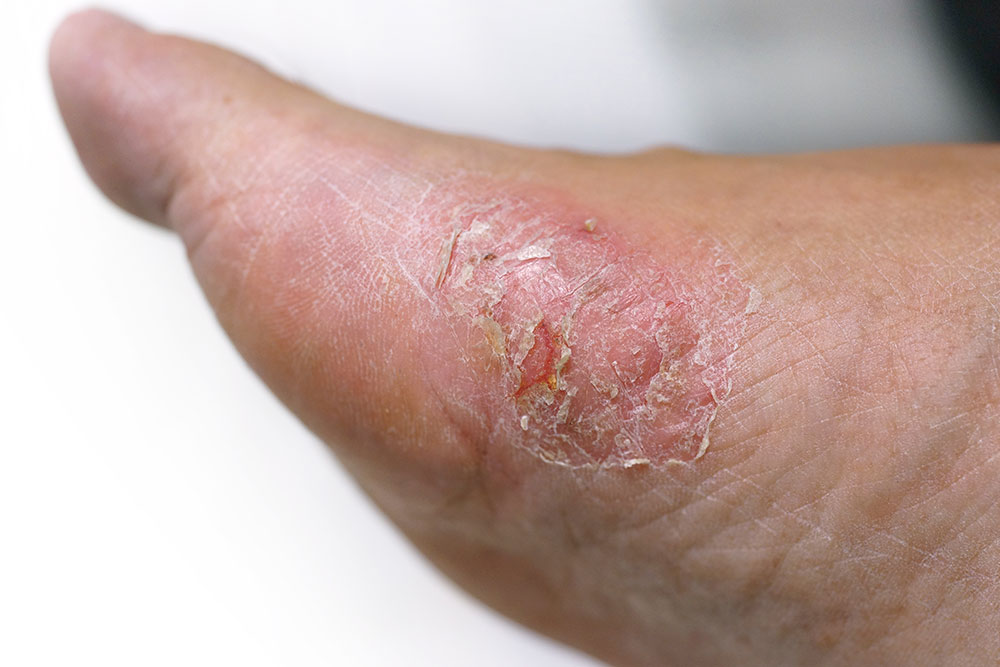
Diabetic Ulcers
open wounds or diabetes groin sores
Diabetes, if remain uncontrolled can cause poor circulation and nerve damage.
And both these factors are responsible for poor wound healing among people with diabetes. And this is particularly true for the feet. These open wounds are commonly referred to as diabetic ulcers.
Prevention:
- A diabetic person must keep a regular check on his or her feet every day for open wounds or sores.
- Get instant medical care in case he or she notices an open sore or wound.
- Discuss with the concerned physician to better control the levels of raised glucose in the blood.
Also Read: Anjeer benefits
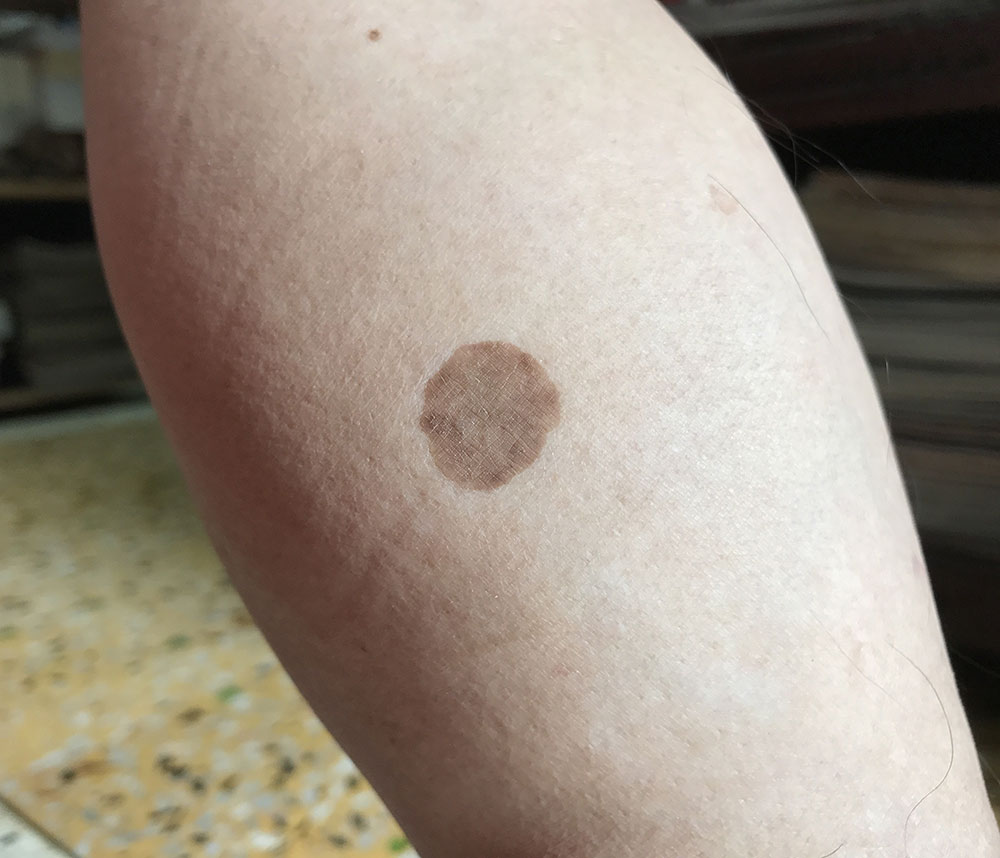
Diabetic Dermopathy or Shiny Spots
This skin problem leads to spots (or lines) on the skin producing a visible depression in the skin. This problem commonly occurs in people with diabetes. It appears on the shins, trunk, arms, thighs, or other body parts. The spots are mostly brown and no signs accompany this condition.
Prevention:
- If a person has been diagnosed with diabetes, get tested.
- Inform the doctor about these spots, in case a person notices them.
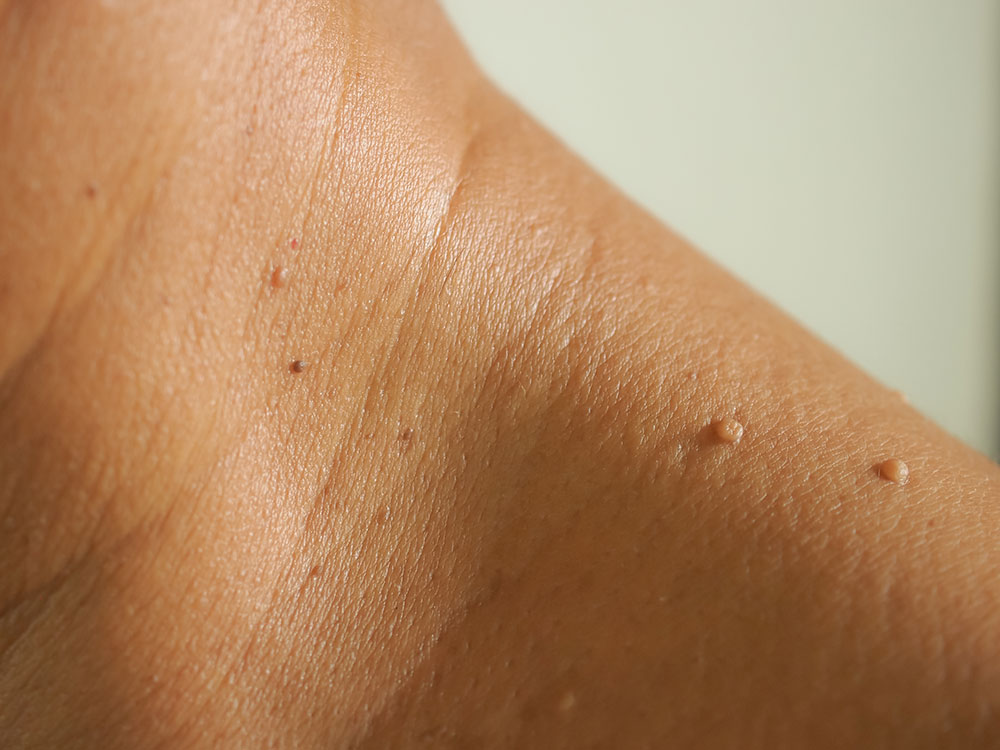
Skin tags
Lots of diabetics suffer from skin tags, which are skin growths hanging from a stalk. While undamaging, having numerous skin tags can be a symptom that the person has an excess of insulin in his or her blood or type 2 diabetes.
Skin tags most commonly occur on the neck, eyelids, groin, or armpit.
Prevention:
- Discuss with a doctor whether or not to get tested for diabetes.
- If the blood sugar levels are high, it’s better to control it.
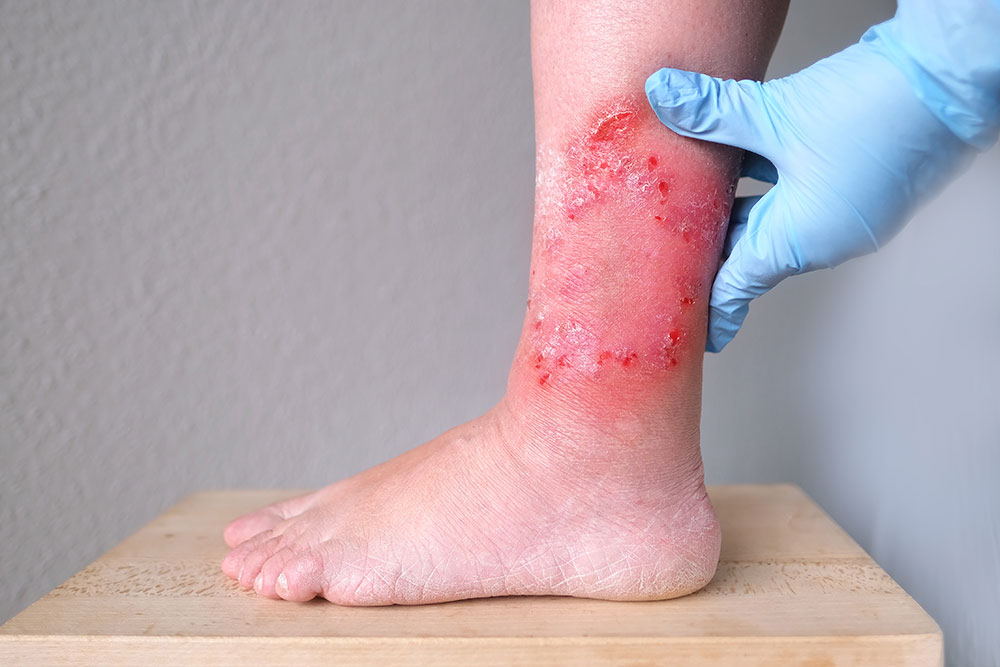
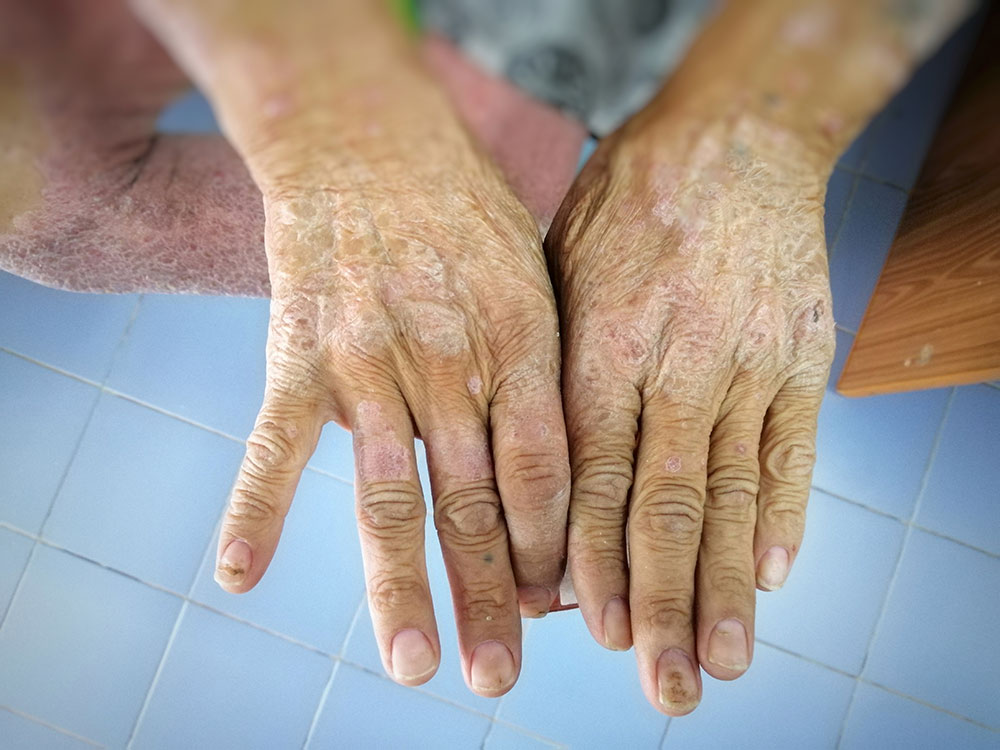
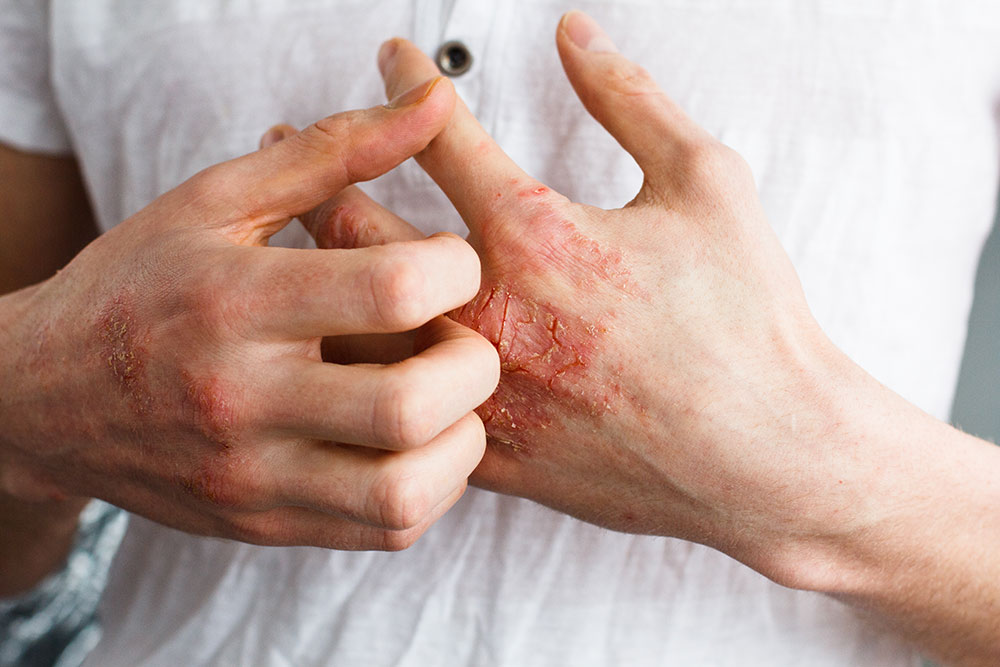
Eczema and Diabetes
In this condition, patches of skin become swollen, scratchy, broken, and hard. Some forms can also result in blisters. The signs of type 2 diabetes rash can be skin flushing, dry, scaly skin, itching, and open sores.
Also Read: Coconut water for diabetes
How to Prevent Skin Problems Caused By Diabetes?
Keeping a tight control on diabetes is most fundamental in preventing skin-associated diabetic complications. Keeping a regular track of blood sugar levels is most vital. Also, skin-associated problems can considerably lessen if a proper skincare routine is followed.
There are a few tips that diabetic people must follow to refrain from skin problems. These tips can be:
- Skin must be kept clean and dry. Warm water and a mild soap must be used while bathing. After washing, ensure a complete rinsing and drying of the body. Remember not to rub the skin; patting the skin to dry can help. Do not forget to dry the areas such as under the arms, breasts, between the toes and the legs.
- Do not take bath in hot water and avoid taking long showers. Never scratch the dry skin and use a moisturizer instead.
- Keep the skin protected from the sun. To do so, make use of good sunscreens or full body clothes.
- Check your body after washing to ensure there are no dry, red, or sore spots that could, later on, become infected.
- Keep the blood sugar levels controlled. It is a must follow the doctor’s recommendations regarding nutrition, exercise, or medicines.
- Avoid getting dehydrated to keep the skin moist and healthy.
- Use a lip balm to avoid chapped lips.
- The cuts should be treated immediately. Soap and water can be used to wash them. The use of antiseptics, iodine, or alcohol must be avoided to clean cuts as they are too harsh.
- It is good to stay away from skincare products available in the market to reduce skin reactions.
- A room humidifier can be used to prevent dry skin when there is a fall in temperature.
- A first-aid kit should always be in hand to look after the hands and feet. It must include gauze pads, paper tape, cleansing towels, soap, antiseptic, and an antibacterial ointment.
- In case, blisters or cuts appear on the skin, never try to break or “pop” the blister. It’s good to wash the area gently with mild soap and warm water. And an antibacterial ointment can be applied to the blister.
- In case, blisters emerge on the feet, it is better to wear a different pair of shoes till healing occurs.
- It’s recommended to check with a doctor if any person experiences rashes after medication intake, rashes near the insulin injection site, any major burn or a cut, or any skin change that does not fade away easily.
Now, easily stamp out skin problems due to diabetes by following these important tips at home.
Summary
Diabetes poses a great impact on almost everybody part initially the skin. Fortunately, a majority of these skin conditions can be managed or easily treated if noticed in their early stages. People with type 1 or 2 diabetes often tend to get skin infections. If any diabetic experiences skin infection, symptoms that may appear can be in the form of dry scaly skin, itchy rash, tiny blisters, or can be a white discharge. Skin problems may erupt on any area of the body between the toes, on the scalp, or around the nails.
Also Read: Healthy lifestyle to prevent diseases
FAQs:
Does diabetes cause dry skin?
If a person is diagnosed with diabetes, he or she is more likely to have dry skin. The raised glucose levels in the blood are the major reason for this.
Can a rash be a sign of diabetes?
Yes, if the rash is infected and if you experience an itchy rash and you scratch it, it may turn into an infection.
Why the skin becomes itchy in people with diabetes?
In diabetics, before the nerve damage occurs, cytokines start circulating in high numbers all around the body. Cytokines are some inflammatory substances responsible for itching. Studies have found that cytokines when an increase in number, diabetic nerve damage happens.
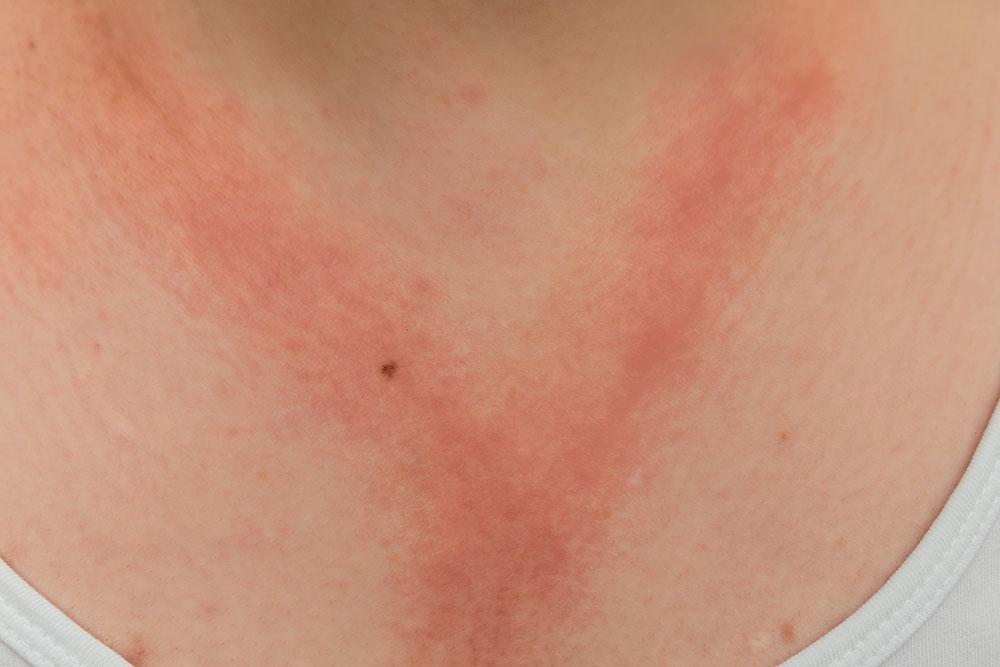
Is there any relation between diabetes and neck rash?
Neck rashes are very common in diabetics. It results in the darkening and thickening of the skin and the skin also gives a velvet feel.
Does high blood sugar cause red face?
If diabetes continues for an extended duration, a red face can occur. Poor blood supply to the skin may lead to certain changes in the fat and collagen lying underneath. Also, the covering skin becomes red and thin.
References:
- https://my.clevelandclinic.org/health/articles/12176-diabetes-skin-conditions
- https://www.aad.org/public/diseases/a-z/diabetes-warning-signs
- https://www.diabetes.org/diabetes/complications/skin-complications
Last Updated on by Dr. Damanjit Duggal
Disclaimer
This site provides educational content; however, it is not a substitute for professional medical guidance. Readers should consult their healthcare professional for personalised guidance. We work hard to provide accurate and helpful information. Your well-being is important to us, and we value your feedback. To learn more, visit our editorial policy page for details on our content guidelines and the content creation process.

 English
English